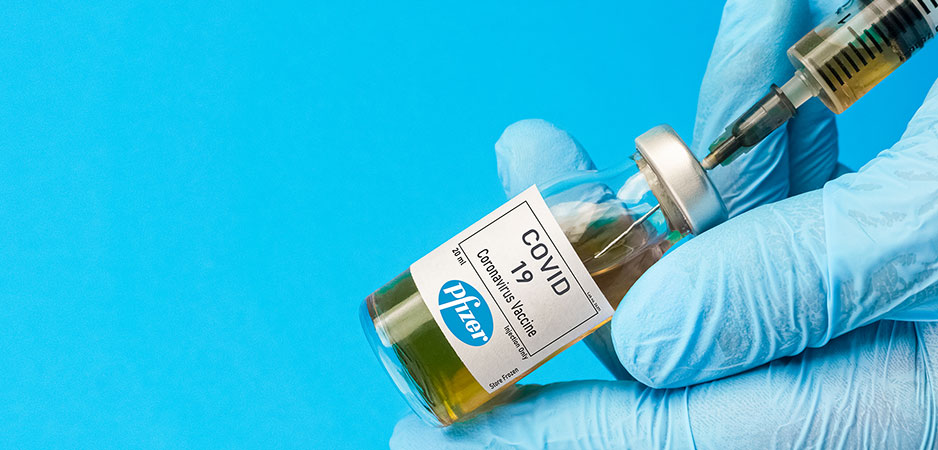
On Monday, November 9, BioNTech, a biotech company owned by a Turkish-German couple, Dr. Ugur Sahin and Ozlem Tureci, together with pharmaceutical giant Pfizer shared some promising news in the wake of the intense race toward eradicating COVID-19. The preliminary but potentially conclusive results of the trial of the mRNA vaccine against the novel coronavirus have sparked flickers of hope around the world. If successful, this will be the world’s first-ever mRNA vaccine. Out of 11 vaccines currently in late-stage trials, only one other company, Moderna, is developing mRNA vaccines against COVID-19, announcing on November 16 that its vaccine also comes with a 94.5% efficacy rate.
Herd Immunity May Be Our Best Hope
Pfizer and BioNTech in a short press release announced that they have conducted a trial on 43,500 volunteers across the US, Argentina, Brazil and Germany, injecting them with two doses of the candidate vaccine at three-week intervals. They presented an analysis of data collected from 94 volunteers who posed as confirmed COVID-19 cases. The ensuing trial, administered just seven days after the second dose, found that the vaccination was effective in more than 90% of volunteers in preventing COVID-19 symptoms and transmission.
Will It Work?
This small group of vaccinated volunteers did not develop any serious side effects. Although almost half of the volunteers in this study were elderly, no data was provided on the efficacy rate among older people, the seriously sick and the highly vulnerable. As of November 8, the trial had enrolled 42% global and 30% US volunteers with racially and ethnically diverse backgrounds. It is not known if this vaccine will work in ethnically different populations that are not part of the trial, and no one can tell how long the immunity might last. More will be revealed about these issues once Pfizer and BioNTech have published their Phase 3 trial data in a scientific peer-reviewed journal.
For this vaccine to be authorized, in accordance with US Food and Drug Administration guidelines, companies need to wait for at least two more months to see if any safety or adverse issues are observed in at least half the trial subjects two months after the last injection. While this vaccine offers huge promise, experts caution that, similar to the flu jab, the first-generation COVID-19 vaccine may not be completely protective.
The biggest stumbling block in the success of mRNA vaccine is proper temperature storage, transport, delivery and continuous temperature monitoring as the vaccine needs to be consistently maintained at around -70˚C or -80˚C. Deviation from these storage requirements reduces both shelf life and efficacy. Such absolute requirements of maintaining a cold chain for the vaccine pose a real challenge in countries with intense heat or poor infrastructure.
Pfizer is currently working on the stability of this vaccine along with other storage and handling issues as well as developing packaging and innovative logistical solutions for various locations around the globe. For example, Pfizer has developed a dry-ice based container in which vaccines can be stored for up to 10-15 days. These containers can be used for transit purposes as well. Alternatively, countries are required to set separate centralized hubs or vaccination centers equipped with ultra-cold freezers where vaccinations can be performed. Success of protein-based vaccines from other ongoing trials will be beneficial to countries with large populations and poor infrastructure.
Who Will Get It?
Pfizer and BioNtech have committed to manufacturing 50 million doses in 2020 and a further 1.3 billion in 2021. This may sound like a lot. However, demand is much higher and over 80% of this supply has been already booked by countries like the US, Canada and Japan as well as the European Union. Ultimately, the statistics suggest that the vaccine may not be available to many other countries before the end of next year.
Another challenge that may be faced by many developing and poorer countries is the cost. While the US and the EU have agreed to a cost of approximately $20 per dose, poorer countries may not be able to afford this vaccine for their entire populations. The world remains hopeful that Pfizer will roll out pricing packages adjusted for different markets. The success of another vaccine out of 11 ongoing trials will not only reduce the cost but will also hasten the process of immunization of a large number of people around the globe.
The success of this or any of the other incoming vaccines is the result of unprecedented and intensified research. A timely and effective partnership between clinicians, scientists and biotech researchers has played a crucial role in its development. It is a proof point that countries will need more laboratories and uninterrupted research funding to have a better understanding of various diseases and become self-sufficient in tackling crises such as COVID-19, with defense mechanisms in place for the protection and survival of the human race.
While the emergence of infectious diseases is unpredictable, it is also important to realize that millions of people across the globe are in a pandemic of their own, affected by cancer, cardiovascular disease, mental health problems or a multitude of other afflictions. Now we have seen what global collaboration between the science, medical and biotech communities can achieve under pressure, there is hope for a similar drive and enthusiasm to come up with solutions that may eradicate many other diseases affecting billions of people worldwide.
*[This article is submitted on behalf of the author by the HBKU Communications Directorate. The views expressed are the author’s own and do not necessarily reflect the University’s official stance.]
The views expressed in this article are the author’s own and do not necessarily reflect Fair Observer’s editorial policy.
Support Fair Observer
We rely on your support for our independence, diversity and quality.
For more than 10 years, Fair Observer has been free, fair and independent. No billionaire owns us, no advertisers control us. We are a reader-supported nonprofit. Unlike many other publications, we keep our content free for readers regardless of where they live or whether they can afford to pay. We have no paywalls and no ads.
In the post-truth era of fake news, echo chambers and filter bubbles, we publish a plurality of perspectives from around the world. Anyone can publish with us, but everyone goes through a rigorous editorial process. So, you get fact-checked, well-reasoned content instead of noise.
We publish 3,000+ voices from 90+ countries. We also conduct education and training programs
on subjects ranging from digital media and journalism to writing and critical thinking. This
doesn’t come cheap. Servers, editors, trainers and web developers cost
money.
Please consider supporting us on a regular basis as a recurring donor or a
sustaining member.
Will you support FO’s journalism?
We rely on your support for our independence, diversity and quality.






Commenting Guidelines
Please read our commenting guidelines before commenting.
1. Be Respectful: Please be polite to the author. Avoid hostility. The whole point of Fair Observer is openness to different perspectives from perspectives from around the world.
2. Comment Thoughtfully: Please be relevant and constructive. We do not allow personal attacks, disinformation or trolling. We will remove hate speech or incitement.
3. Contribute Usefully: Add something of value — a point of view, an argument, a personal experience or a relevant link if you are citing statistics and key facts.
Please agree to the guidelines before proceeding.